
When travelling during long haul flights, it can place a unique set of physiological demands on our body and for many travellers, these demands can accumulate into significant discomfort or even medical risk.
Prolonged immobility, disrupted circadian rhythms, low cabin humidity and cramped seating can contribute to an increased risk of venous thromboembolism (VTE), jet lag, menstrual irregularities and overall general travel fatigue.
UK guidance from NaTHNaC, NHS, NICE and the British Society for Haematology (BSH) continue to highlight the importance of a structured risk assessment and tailored prevention strategies when travel healthcare professionals carry out their consultations. Yet these topics can receive less attention in travel consultations when the main focus can be concentrated on vaccines or destination‑specific risks.
For travel‑health professionals, integrating these issues into routine practice can help improve traveller safety and comfort.
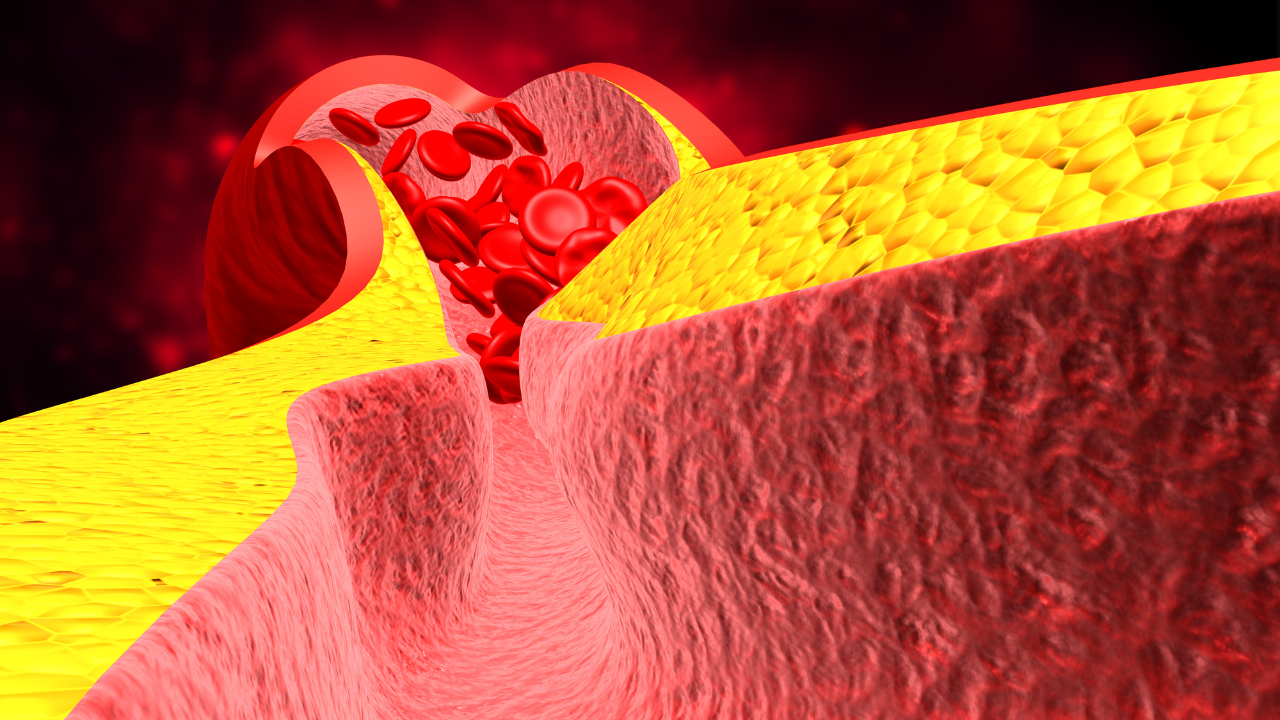
VTE, which includes deep vein thrombosis (DVT) and pulmonary embolism (PE), can occur when prolonged immobility slows venous return from the lower limbs, allowing blood to pool and clot.
The pressure exerted by aircraft seating can further impede blood flow and although the risk for healthy travellers is potentially low, it is estimated at around 1 in 6,000 for flights over four hours.
The risk can increase with longer journeys and multiple flights in close succession. West Suffolk NHS Foundation Trust notes that the risk rises sharply on flights over 16 hours, with estimates of around 1 in 1,200 for very long journeys.
Travellers with additional risk factors face a significantly higher likelihood of VTE. These include:
NaTHNaC also highlights older age and certain cardiac conditions as relevant risk factors. These considerations show how important it is to conduct a thorough patient assessment during pre‑travel consultations.

A comprehensive medical history is central to identifying travellers who may be at increased risk during long‑haul flights. It is the healthcare practitioner’s chance to discuss with their patient, precautionary measures, which can reduce their patient’s risk as much as possible. Travel healthcare practitioners should advise:
Reviewing the patient’s full medication list is essential, as many travellers may take anticoagulants for conditions such as atrial fibrillation or previous VTE. While travel‑health professionals can provide general information about these medicines, it is important to note that any questions relating to their patient’s medications, their dose timing or regimen adjustments must be referred back to the patient’s prescribing clinician.
Understanding the traveller’s itinerary is equally important. Flight duration, stopovers, seat selection and the frequency of long‑haul travel all influence their risk.
These details help travel healthcare professionals tailor advice and identify when it’s in the best interest of the patient to seek further advice from their GP (General Practitioner) or specialist practitioner. Travel insurance should also be discussed, with emphasis on the need for full disclosure of medical conditions to avoid invalidating cover.
Anticoagulants are widely prescribed for a range of cardiovascular and thrombotic conditions. Travellers taking these medicines (or any other medications) should be encouraged to:
Again, travel health professionals should reinforce to the patient, the importance of consulting their prescribing clinician if the traveller has concerns about flying, potential medication interactions or dose timings.
Hydration also plays a key role. Low cabin humidity increases fluid loss, so travellers should be advised to drink water regularly and limit alcohol and caffeine, both of which can contribute to dehydration. Sedating medications should be avoided unless clinically necessary, as they may reduce mobility.
Compression hosiery is another effective preventive measure for travellers at moderate risk. Properly fitted, medical‑grade stockings can reduce the likelihood of VTE by supporting venous return. Travel healthcare practitioners should explain the difference between medical‑grade compression and retail “flight socks”, emphasising the importance of correct sizing and appropriate use.
Pharmacological prophylaxis, such as low molecular weight heparin, may be recommended for high-risk travellers, but only by a clinician with prescribing authority and full access to the traveller’s medical history.
Travel-health professionals should avoid initiating or suggesting pharmacological prophylaxis independently.

Jet lag occurs when the body’s internal circadian rhythm becomes misaligned with the destination time zone. Symptoms may include:
These effects can become worse when crossing multiple time zones, especially on eastbound flights.
Circadian disruption can also temporarily affect the menstrual cycle. Some travellers may notice temporary changes in their menstrual cycle due to factors such as time-zone changes, disrupted sleep and travel-related stress.
Travellers may experience early or delayed periods, heavier bleeding or more intense premenstrual symptoms. Clinicians should reassure travellers that short-term changes can occur and usually settle, and encourage travellers to pack adequate menstrual products and analgesia for severe cramping.
In the UK, one medication that may be considered for delaying a period is Norethisterone. Clinicians may consider it for people who want to postpone bleeding for a short time, especially while on holiday.
Norethisterone works by keeping progesterone levels high, which prevents the uterine lining from shedding. However, there are a few important key points to remember:
It is important to note that any medication affecting hormones must be considered carefully in the context of VTE risk, especially for long‑haul flights, therefore only a prescribing clinician can decide:
As a travel healthcare practitioner, your role when conducting travel health consultations is to provide general information, explore the traveller’s goals, and signpost them to their GP or sexual health provider for personalised advice.
Light exposure is one of the most effective tools for managing jet lag. Travellers can help reset their circadian rhythm by seeking morning light when travelling east and evening light when travelling west. Minimising unwanted light exposure through the use of sunglasses or eye masks can also support adaptation. Sleep strategies can further ease jet lag symptoms such as:
Non‑pharmacological sleep aids, including earplugs, eye masks and neck pillows, may also improve comfort. Melatonin may be appropriate for some travellers and is licensed in the UK for short-term treatment of jet lag in adults, although it is not always routinely prescribed on the NHS. Suitability should be assessed by a clinician.

Comfort items such as travel pillows and blankets can also improve rest and reduce fatigue.
Travel fatigue is influenced by:
Encouraging travellers to stay hydrated, eat light meals, wear loose clothing and use moisturiser or lip balm can help ease discomfort. Comfort items such as travel pillows and blankets can also improve rest and reduce fatigue.

Clinicians should tailor medical kit recommendations to the traveller’s health status, their destination and itinerary.
A well-prepared travel medical kit can support self-care and symptom management during long-haul flights, contributing to a more comfortable journey. Clinicians should tailor medical kit recommendations to the traveller’s health status, their destination and itinerary. Items can include:

Embedding discussions about VTE prevention, jet lag, menstrual health and fatigue into routine consultations ensures that travellers receive holistic, evidence‑based advice.
Normalising these conversations helps travellers feel more prepared and confident. Providing written resources or signposting to reputable sources can reinforce verbal advice and support behaviour change. Encouraging travellers to seek GP or specialist input when needed ensures safe, coordinated care.
Long‑haul flights can present a range of preventable risks that can significantly affect the traveller’s wellbeing. By integrating these topics into routine consultations, travel‑health professionals can enhance safety, comfort and confidence for their travellers.
Thorough history‑taking, medication review and appropriate referrals remain central to safe practice. As long‑haul travel continues to grow, these conversations are essential components of high‑quality travel‑health care.
Giving you written and video content to answer all your questions on primary care education from Phlebotomy to Travel Health.
Subscribe now to be kept updated with our latest posts and insights.
Start typing to search courses, articles, videos, and more.
Notifications