
Cervical cancer is one of the most preventable and treatable forms of cancer. In the UK, proactive measures have been implemented to reduce the impact of cervical cancer through cervical screening programmes and the introduction of the national Human Papillomavirus (HPV) vaccination programme. This has been shown to be a true game-changer, significantly reducing the incidence of cervical cancer and its associated morbidity and mortality. However despite this, cervical cancer remains a significant public health concern in many countries worldwide. Sadly, the burden of this disease falls disproportionately on low and middle-income countries, where access to healthcare and education remains limited.


Cervical cancer is the uncontrolled growth of abnormal cells in the lining of the cervix. It is a type of cancer that is predominantly caused by persistent infection with high-risk Human Papillomavirus (HPV). HPV is found in 99% of cervical cancer cases, with subtypes HPV 16 and 18 accounting for at least two-thirds of cases.
HPV is the most common viral infection of the reproductive tract and is primarily transmitted through sexual contact. It is thought most sexually active women and men will become infected at some point in their lives, some even multiple times. More than 90% of those infected eventually recover, however around 10% of all infections persist. This can lead to the development of precancerous lesions, which typically take between 1-10 years to develop.
Every year, it is estimated that globally there are around 600,000 new cases of cervical cancer, with it leading to the loss of lives of over 340,000 women. Cervical cancer accounts to being the 4th most common cancer amongst women worldwide.
In the UK, according to Cancer Research UK, cervical cancer is believed to affect 1 in every 142 females in the UK in their lifetime. It is the 14th most common cancer in females, with around 3,200 new cases every year. This leads to around 850 deaths in the UK each year; more than 2 every day.
Cervical cancer primarily affects sexually active women aged 30-45, with females aged 30-34 having the highest incidence rates. However, a second, smaller peak occurs in women over the age of 80, who are less likely to have benefited from cervical cancer screening throughout their lives. Cervical cancer is rare in those under 25.


Cervical cancer is one of the most preventable and successfully treatable forms of cancers. The National Institute for Health and Care Excellence (NICE) guidance for HPV and cervical cancer states that prevention of cervical cancer should include advice on:
According to NICE guidance, cervical cancer should be suspected if a woman has:
Individuals with possible symptoms should be encouraged to seek medical advice as soon as possible, regardless of what their age is.
It is thought that exposure to HPV infection from an early age can increase risk factors to development of cervical cancer. This is why it is important to vaccinate boys and girls at a young age before they are likely exposed. Other factors that can increase risk can also include an impaired immune response such as solid organ transplant or Human Immunodeficiency virus (HIV). Data shows that women living with HIV are actually up to six times more likely to develop cervical cancer in their lifetime in comparison to women without HIV.
The 17th of November is the World Health Organization’s (WHO’s) Cervical Cancer Elimination Day of Action. This annual event serves as a reminder of the importance of cervical cancer prevention, early detection and treatment, and is an opportunity to reflect and consider what more we can be doing to help reduce the burden of the disease.
In 2020 WHO launched a global strategy to accelerate the elimination of cervical cancer. In this strategy they outlined targets for HPV vaccine uptake in adolescent girls, cervical screening uptake, and the need for early access to high-quality cancer treatment.
“This is a historic moment for global health. It marks the first time that the world has committed to eliminating a cancer.”
WHO Director-General, Dr Tedros Adhanom Ghebreyesus (17 November 2020)
The strategy aims to achieve the 90-70-90 targets by 2030, in which 90% of girls are fully vaccinated against HPV by the age of 15, 70% of women have access to high-performance cervical cancer screening tests by the age of 35 and again by the age of 45, and 90% of women with cervical cancer have adequate access to quality treatment and management.
As the only Non-Communicable Disease (NCD) that can be truly eradicated, cervical cancer will move the world closer to achieving the WHO’s Sustainable Development Goal 3.4. Reducing the illness will have a major impact on the goal of a third fewer premature deaths by 2030.
“Reduce by one third premature mortality from non-communicable diseases through prevention and treatment and promote mental health and well-being“
WHO’s Sustainable Development Goal 3.4
Improving awareness of the disease, access to vaccines and ensuring efficient screening practices can all help to lower the high death rate that exists worldwide. It is hoped that this will mean the the median cumulative number of cervical cancer deaths averted by 2030 will be 300,000, 14 million by 2070, and more than 62 million by 2120.
Sadly few diseases are more representative of global inequalities than cervical cancer. 2020 saw about 90% of new cases and deaths take place in low and middle-income nations globally. Whilst high-income countries have programmes in place that allow girls (and in some countries boys too) to be vaccinated against HPV and women to be screened and treated on a regular basis. In low and middle-income countries, access to these preventive measures is limited. Cervical cancer is often frequently not detected until it has progressed and symptoms appear. Furthermore, access to treatment for cancerous lesions, for example surgery, radiotherapy, and chemotherapy, can also be more limited in these countries, resulting in a higher rates of death.
HPV vaccination uptake globally has up until now also been markedly low even though HPV vaccines have been authorised since 2006. According to the WHO, in 2020, global coverage for girls in the target age was only 13%, far off the 90% target. Although we are slowly making progress, with the help of organisations such as Gavi, UNICEF and the WHO more countries are introducing the HPV vaccine into their national programmes.
In the UK, The National Health Service (NHS) provides a comprehensive cervical screening programme for eligible individuals. Since it commenced, the number of women dying from cervical cancer has been cut in half. It is estimated that around 4500 lives every year are saved due to the programme.
Cervical screening is typically recommended for women and people with a cervix between the ages of 25 and 64, with invitations sent by the NHS every 3-5 years.
Those age 65 and up are invited if a recent cervical cytology sample is abnormal, or if they have not had a cervical screening test since the age of 50 and request one.
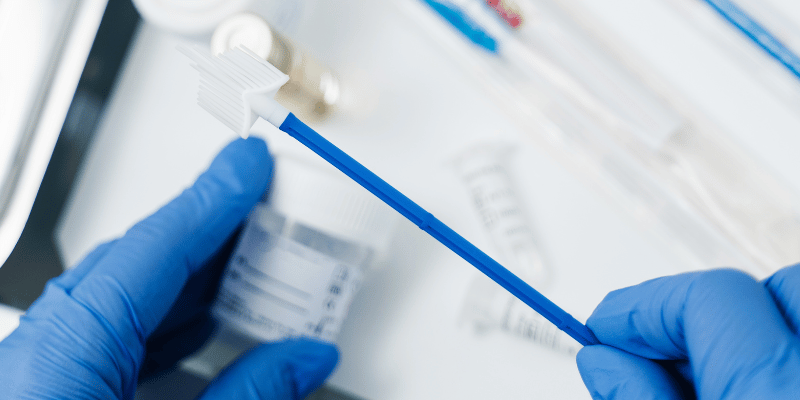
Cervical screening involves a quick and simple process where a sample of cervical cells is obtained during a pelvic examination and sent for laboratory analysis. The UK transitioned to primary HPV testing from cytology screening in 2019 as it was shown to be more effective at detecting high-risk HPV types associated with cervical cancer.
If HPV is detected, then liquid cytology testing is used to look for abnormal changes in the cells. Repeat testing is advised after a year if no abnormal cells are found. If abnormal cells are detected, further tests, such as a colposcopy are then performed. A colposcopy will help to diagnose cervical intraepithelial neoplasia (CIN) which helps to differentiate high-grade lesions from low-grade abnormalities in those with abnormal cytology. Lesions can be treated by excising or ablating the affected tissue during the precancerous phase.
For those diagnosed with cervical cancer, it is important healthcare professionals involved in their care offer compassionate and comprehensive care and that patients receive the support and information they need to make informed decisions about their treatment options.
If caught early enough to treat, the disease can be cured even if it develops into cancer. For those diagnosed with cervical cancer a variety of treatment methods are available. Surgery, radiotherapy, and/or chemotherapy may be necessary as part of the treatment if the lesions have become cancerous. Palliative care and appropriate treatment can be used to minimise pain and suffering in cases of late-stage cancer diagnosis.

Cervical screening has huge benefits, it means that cervical cancer can be detected early and can prevent around 70% of cervical cancers from developing in the first place. Since the implementation of formal screening programmes in high-income countries 30 years ago, the incidence and mortality of cervical cancer have more than halved.
As healthcare professionals we can play a crucial role in the promotion of regular cervical cancer screening, emphasising the importance of early detected in increasing treatment success rates. We should ensure that eligible patients are aware of these invitations and the importance of participating.
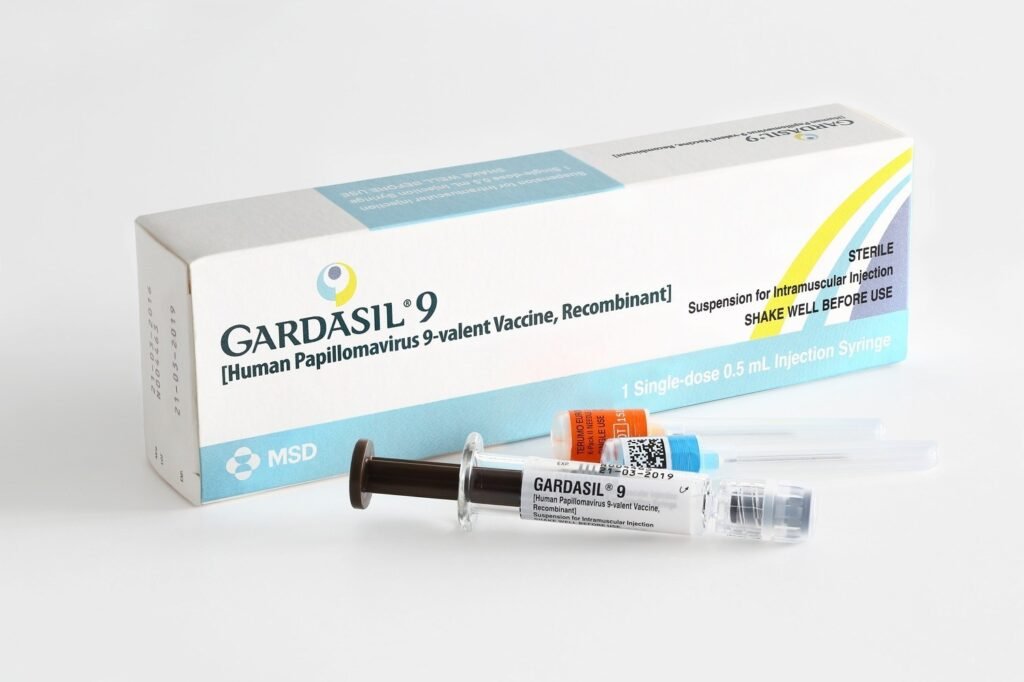
In the UK, the national HPV vaccination programme was introduced in September 2008. Initially only girls aged 12-13 were offered the vaccination, however since it’s introduction the programme has been expanded to now include all boys aged 12-13 since 2019. The HPV vaccine programme was also rolled out in 2018 to include gay, bisexual and other men-who-have-sex-with-men (GBMSM) up to the age of 45. Currently Gardasil©9, is used as part of the UK vaccination programme which protects against 9 types of the most common cancer causing HPV types.
Individuals remains eligible for vaccination up until their 25th birthday for:
In 2022 the WHO announced that the vaccine schedule could move from the recommended 2 doses to a 1 dose schedule, this was recently implemented in the UK in September 2023. Research showed that a 1 dose schedule was comparable in effectiveness to the 2 or 3 dose schedule (although 3 doses is currently still used in those who are immunosuppressed and 2 doses for GBMSM aged 25-45). It is anticipated that having a single dose schedule will be less expensive, less resource intensive, and easier to administer, ultimately helping us to meet our global targets for vaccination rates. You can read more about the changes in the UK Health Security Agency’s (UKHSA’s) HPV Vaccination programme Changes from September 2023 Letter.
The NHS HPV vaccination programme in England has been shown to significantly reduce HPV infections and cervical cancer rates in vaccine-eligible women, with the strongest effects seen in those offered vaccination at younger ages. A study published in The Lancet in 2021 found that the rates of cervical cancer were 87% lower in young women who had been eligible for vaccination when they were 12 to 13 years old, compared to young women who had not been offered vaccination.
The HPV vaccine has also been linked to a significant decrease in the number of precancerous cervical lesions, such as cervical dysplasia. According to the study, as of mid-2019, the HPV programme had averted approximately 17,200 pre-cancers and 450 cancers.
However it is not just cervical cancer rates that have seen a benefit from the HPV vaccine. HPV vaccination also protects men and women against genital warts, other genital cancers and some head and neck cancers. Not only that but the vaccine’s widespread use has contributed to herd immunity, protecting even those who may not be eligible for vaccination. This is a significant public health benefit.
Several countries worldwide with strong vaccination programs have also reported a remarkable reduction in cervical cancer cases among vaccinated populations. In some areas, cervical cancer may become a rarity rather than a common occurrence. This decrease in infection rates is a critical step in reducing the risk of cervical cancer. As healthcare professionals we can help to encourage HPV vaccination among eligible populations. We must inform young people and their parents and caregivers about the importance of vaccination and ensure that vaccination services are accessible to all.
It is known that certain groups of women have been reported to have low cervical screening rates, such as some ethnic minority groups or women from foreign countries. Currently around one third of women invited do not take up the offer. Furthermore, women in the most deprived groups are less likely to attend screening but they are more likely to have high-risk HPV and an increased risk of being diagnosed or dying from cervical cancer. According to data from Cancer Research UK, the incidence rates of cervical cancer in England are 65% higher in the most deprived areas compared with the least.
Covid-19 also brought disruption to school vaccination programmes and the latest data from 2021-22 shows that rates of HPV vaccination in the UK are yet to return to pre-pandemic levels. However other factors that can affect vaccination rates include knowledge, attitudes, practices, understanding and socio-cultural norms.

The HPV vaccine has been an incredible success story in the world of cervical cancer prevention alongside the implementation of cervical screening programmes.
NHS England recently announced its aim to eliminate cervical cancer by 2040. This makes England amongst one of the first countries in the world to set this elimination ambition within the next two decades. It is hoped this can be achieved by raising cervical screening uptake rates and by making it as simple as possible for people to receive the lifesaving HPV vaccine through targeted outreach programmes and offering vaccinations in more convenient settings. They also hope to expand the functions of the NHS app to enable more individuals to be able to access their vaccination records to identify any gaps in their history and book appointments at the click of a button.
As healthcare professionals we are at the forefront of this effort, and we play a crucial role in educating patients about the risks of cervical cancer, the benefits of screening, and the importance of HPV vaccination.
We should feel confident to address any concerns or misconceptions our patients may have. We should also aim to actively contribute to improving screening and vaccination rates and address health inequalities and disparities, so that all eligible individuals have access to screening and vaccination services. By working collaboratively, we can continue to reduce the burden of cervical cancer and bring us closer to its goal of elimination. Let’s aim to make cervical cancer a thing of the past and ensure that everyone has the opportunity to live healthy, cancer-free lives.
Why not reflect on your learning from this article as part of your continuing professional development (CPD). Click below to fill out a short form which can be emailed to yourself for your own records.

Giving you written and video content to answer all your questions on primary care education from Phlebotomy to Travel Health.
Subscribe now to be kept updated with our latest posts and insights.
Start typing to search courses, articles, videos, and more.