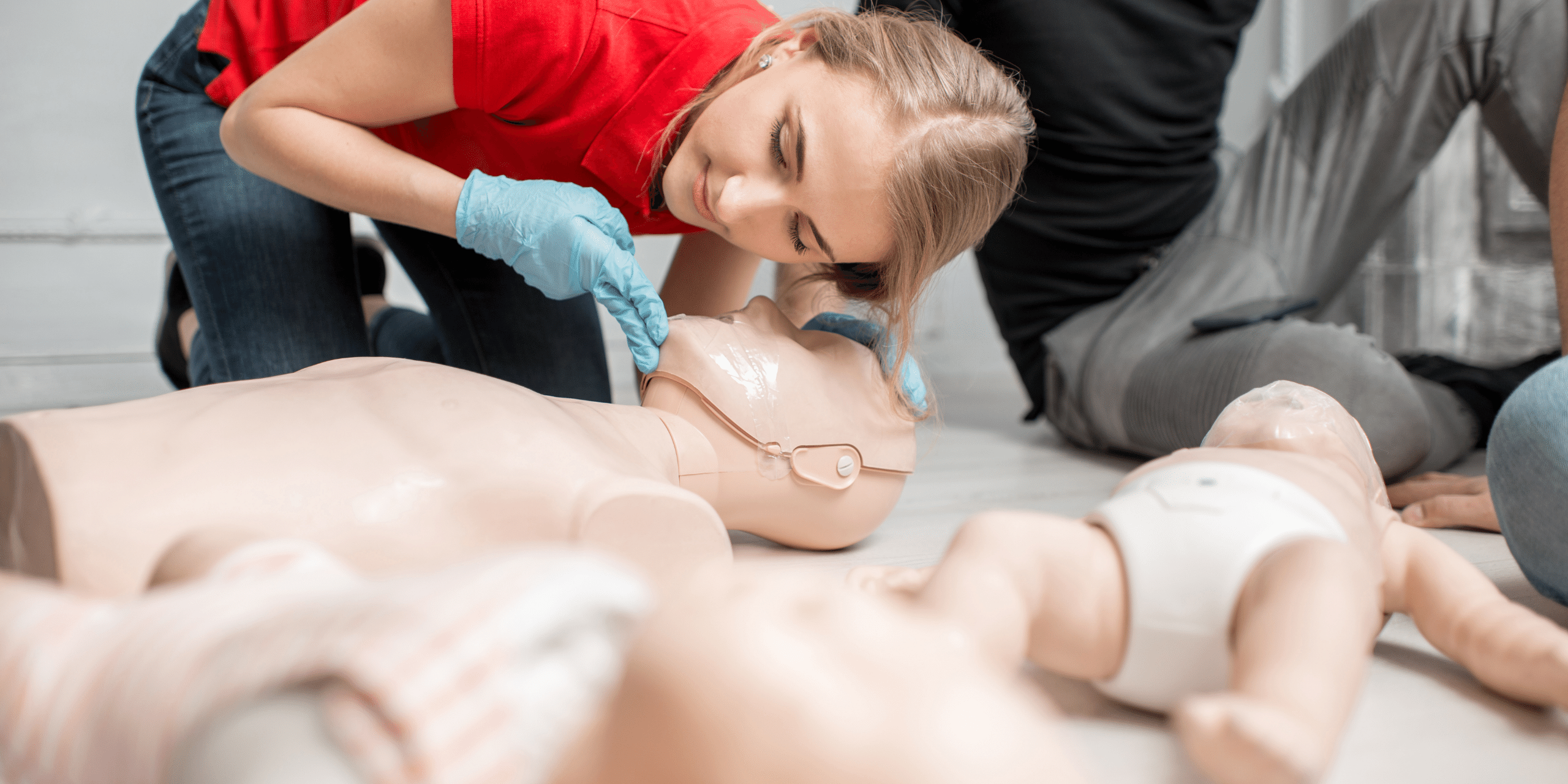
Although rare, paediatric resuscitation episodes will inevitably be an extremely stressful situation for all involved. As the health care professional in a paediatric BLS situation, everyone will be looking to you for a confident and methodical approach to the situation. Those health care professionals that do not usually come in to contact with children in their professional role may find this particularly daunting.
I am going to cover a recent key change to the Resuscitation Council (UK) guidelines in this blog post. If you work with children in your professional role, you should ensure you are up to date with your training on Paediatric BLS. If you do not work with children in your professional role, at the very least you should familiarise yourself with the Resuscitation Council (UK) guidelines. (Click on the algorithm below to take you there).
We have all been taught for years to treat an under 1 year old as an infant and anyone over one that looks like a child (up to around puberty) we treat as child for the purposes of paediatric BLS. For those that look like they have reached puberty, we follow the adult protocol.
So has this changed? The answer is yes and no.
The Resuscitation Council Guidelines 2021 now state the following age categories:
This is where there has been a subtle but important change to paediatric BLS. Previously if we were faced with a young person and we thought they looked more adult like, then we were encouraged to use the adult protocol. This has now shifted in the other direction.
The guidelines state:
The differences between adult and paediatric resuscitation are largely based on differing aetiology. If the rescuer believes the victim to be a child then they should use the paediatric guidelines. If a misjudgement is made, and the victim turns out to be a young adult, little harm will accrue as studies of aetiology have shown that the paediatric causes of arrest continue into early adulthood.
The majority of paediatric cardiac arrests are caused by hypoxaemia or ischaemia and oxygen reserves are most often depleted by the time arrest occurs. Therefore, with evidence showing that often the same causes of paediatric arrest continues in to early adulthood, a young adult will most likely be oxygen depleted at time of arrest. If you would like to read more on the evidence base behind the changes in the guidance, the European Resuscitation Council publishes this alongside the guidelines.
The focus of the change has been to ensure that those who are likely to be in arrest due to hypoxaemia receive rescue breaths as soon as possible. However the guidelines for other practical aspects of resuscitation in children should be followed specifically:
Compress the chest by at least one-third of its depth, approximately 4 cm for an infant and approximately 5 cm for an older child. Use both thumbs or two fingers for an infant under 1 year; use one or two hands for a child over 1 year as required to achieve an adequate depth of compression
In larger children, or for small rescuers, effective compressions may be achieved more easily by using both hands with the fingers interlocked.
If possible, use an AED with a paediatric attenuator in infants and children below 8 years (energy reduced to 50-75 J). If this is not available, use the standard AED (for all ages).
The Anaphylaxis guidelines have also been updated in 2021 and these changes will be covered in a separate blog post. However in specific regard to pediatric anaphylaxis there is now a specific dose of adrenaline included for children below 6 months of age:
The management of the choking child with the sequence of reversing partial or complete obstruction of the airways remains unchanged. Follow the current Paediatric BLS Guidelines (Resuscitation Council 2021) for exact procedures.
The Resuscitation Council (UK) guidelines state:
Those trained only in adult BLS (may include healthcare providers and members of the public) who have no specific knowledge of paediatric resuscitation, should use the adult sequence they are familiar with, including the paediatric modifications if possible.
Are you due your annual update training? We have a range of different courses in both adult and paediatric BLS available at Health Academy.


Giving you written and video content to answer all your questions on primary care education from Phlebotomy to Travel Health.
Subscribe now to be kept updated with our latest posts and insights.
Start typing to search courses, articles, videos, and more.